Chronic Urticaria
Chronic urticaria (CU) is defined as wheals (hives), angioedema (swelling), or both that have been continuously or intermittently present for at least six weeks. The term urticaria is another word for itching, also known as pruritis. While most patients with chronic urticaria wind up seeing an allergy/immunology specialist, many begin the evaluation of their condition at their primary care doctor’s office. It is estimated that 500,000 people in the U.S. have CU, or about 0.23% of the population. It affects people at any age but is most commonly seen in women over 40 years of age. It can have substantial negative effects on daily life, including physical and emotional functioning and sleep disorders. The degree of life impairment is on a par with those with coronary artery disease who are awaiting bypass grafting.
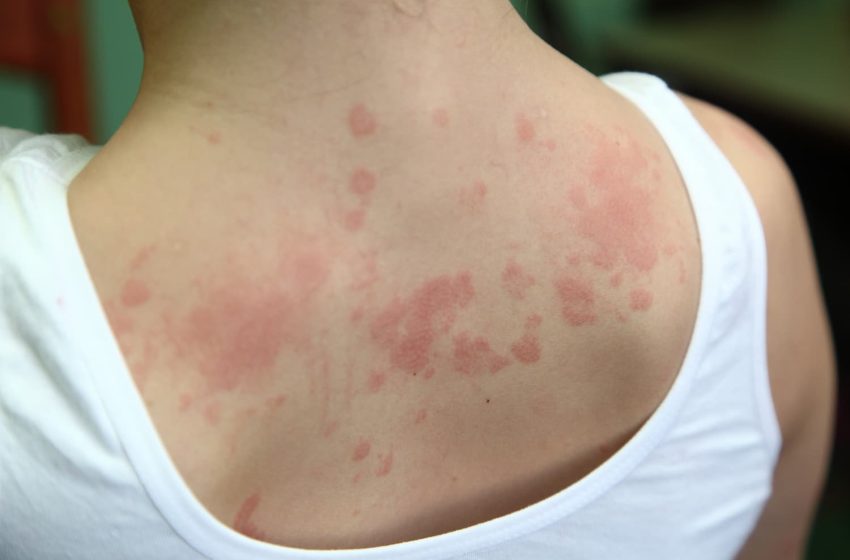
The underlying cause of CU appears to be inflammation. Starting with the release of mast cells, which contain histamine, there is an inflammatory cascade that releases prostaglandins, leukotrienes, eosinophils, etc. that result in leakage of plasma into and below the skin causing angioedema. In acute urticaria, there is a known causative agent, often a medication the patient is taking. In CU, there is no known cause. In rare cases, an underlying systemic disorder is to blame, such as rheumatologic disease, infection, or hematologic cancer. CU is characterized by pruritic wheals with surrounding erythema (redness) that occur on any part of the body. The erythema may be more difficult to discern on darker-skinned individuals. The itching can be severe, however scratching the affected areas only worsens the swelling and itching. When the angioedema, or swelling, occurs it is mainly on the face, torso, or hands. Evocative tests may be performed to confirm the diagnosis. The two most common tests are dermatographia (“skin writing”) and cholinergic urticaria. In dermatographia, using a firm object like a tongue depressor to stroke the skin will result in redness and swelling of the stroked area, usually within five minutes. Cholinergic urticaria results in redness and swelling after heat application to the skin, which explains why vigorous exercise may provoke CU symptoms.
Management of CU includes lifestyle changes as certain factors may lower the threshold for breakthrough episodes, including alcohol, opiates, stress, and the use of NSAIDS. Episodes have also been seen to occur with the start of a menstrual period. Treatment begins with antihistamines (Benadryl) and mast cell stabilizers (montelukast). More severe or resistant cases may require short courses of corticosteroids (prednisone), while resistant cases can be prescribed omalizumab (Dupixent, Fasenra, Xolair), an IgE blocker. IgE is the immunoglobin associated with allergies and allergic diseases like asthma. Unfortunately, CU can be resistant to treatment, as studies have shown that only about 35% of patients with CU are symptom-free after one year of treatment.
Please direct questions and comments to editor@rockawaytimes.com


