Hairum Scareum

By Peter Galvin, MD
Today’s column is from the category of you’re never too old to learn something new. I came across a case study in a medical journal of a syndrome I was not familiar with. The case involved an 80-year-old man who presented to the ER with fever and shoulder pain. To make a long story short, he wound up having a shoulder arthroscopy and his blood cultures, done on admission, grew MSSA, or methicillin-sensitive Staphylococcus aureus. He was placed on antibiotics and a week after hospitalization, his tongue turned black (see photo). He had no symptoms and denied using chewing tobacco, cigarettes, illicit drugs, or alcohol.
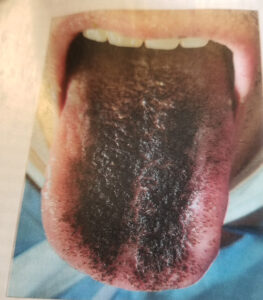 It turned out that he was diagnosed with black hairy tongue (lingua villosa nigra). I don’t know about you, but if my tongue or my patient’s tongue looked like the photo, shall I say, I would be a bit alarmed. Black hairy tongue is characterized by discoloration of the dorsal (upper) surface of the tongue accompanied by hypertrophied (enlarged) papillae that appear like hair growth on the tongue. Although the tongue typically appears black, it may take other shades like brown, yellow, green, or blue. Most people with this have no symptoms, however some will present with halitosis (bad breath), dysgeusia (altered taste), gagging, nausea, or pain or burning of the tongue. The exact cause is unknown, but it is caused by defective desquamation (skin shedding) of the keratinized layers of the tongue, leading to a skin accumulation that forms bumps, or papillae. These papillae accumulate bacteria, fungi, and residue from food, coffee, tea, and tobacco.
It turned out that he was diagnosed with black hairy tongue (lingua villosa nigra). I don’t know about you, but if my tongue or my patient’s tongue looked like the photo, shall I say, I would be a bit alarmed. Black hairy tongue is characterized by discoloration of the dorsal (upper) surface of the tongue accompanied by hypertrophied (enlarged) papillae that appear like hair growth on the tongue. Although the tongue typically appears black, it may take other shades like brown, yellow, green, or blue. Most people with this have no symptoms, however some will present with halitosis (bad breath), dysgeusia (altered taste), gagging, nausea, or pain or burning of the tongue. The exact cause is unknown, but it is caused by defective desquamation (skin shedding) of the keratinized layers of the tongue, leading to a skin accumulation that forms bumps, or papillae. These papillae accumulate bacteria, fungi, and residue from food, coffee, tea, and tobacco.
Factors associated with black hairy tongue include certain behaviors like smoking or chewing tobacco, alcohol use, heavy black tea consumption, illicit drug use, poor dental hygiene, and excessive use of oxidizing mouth washes that contain sodium perborate, sodium hydroxide, and hydrogen peroxide. Medications associated with it include many antibiotics, some antipsychotics (olanzapine and chlorpromazine), and some chemotherapeutic agents. Those at risk for developing the syndrome include those who are edentulous or have HIV, advanced cancer, graft-vs-host disease, trigeminal neuralgia, amyotrophic lateral sclerosis, chronic xerostomia (dry mouth), or who have received radiation therapy to the head or neck. It has also been reported in cases of COVID-19.
While the exact prevalence of black hairy tongue is unknown, some population estimates put it at 1.2% to 11.3%. It is three times more common in men, which may be due to their higher rates of cigarette smoking and poor oral hygiene. The prevalence also increases with age, especially after age 60 years. It should be differentiated from pseudo-black hairy tongue, a condition where the tongue is stained by medications (e.g., bismuth subsalicylate [Pepto-Bismol] and minocycline), chemicals, or food dyes. Aside from cosmetic concerns, black hairy tongue is benign. Treatment includes eliminating the causative agent, if any, brushing the tongue with a soft toothbrush or tongue scraper, and improving oral hygiene. It generally resolves on its own, as it did in the patient in the case study.
Please direct questions and comments to editor@rockawaytimes.com


